Urinary Tract Infections (UTIs) are one of the most common health issues affecting millions of people worldwide, particularly women. While many UTIs are mild and treatable, ignoring the infection can lead to complications. Understanding UTI symptoms, UTI causes, and the best UTI treatment options is essential for early diagnosis and prevention.
In this article, we’ll explore everything you need to know about UTIs from what they are to how you can prevent them.
What is a UTI?
A UTI (Urinary Tract Infection) is an infection that affects any part of the urinary system, including the kidneys, bladder, ureters, or urethra. Most cases involve the bladder and urethra.
UTIs are more common in women due to anatomical factors the female urethra is shorter, making it easier for bacteria to enter the bladder.
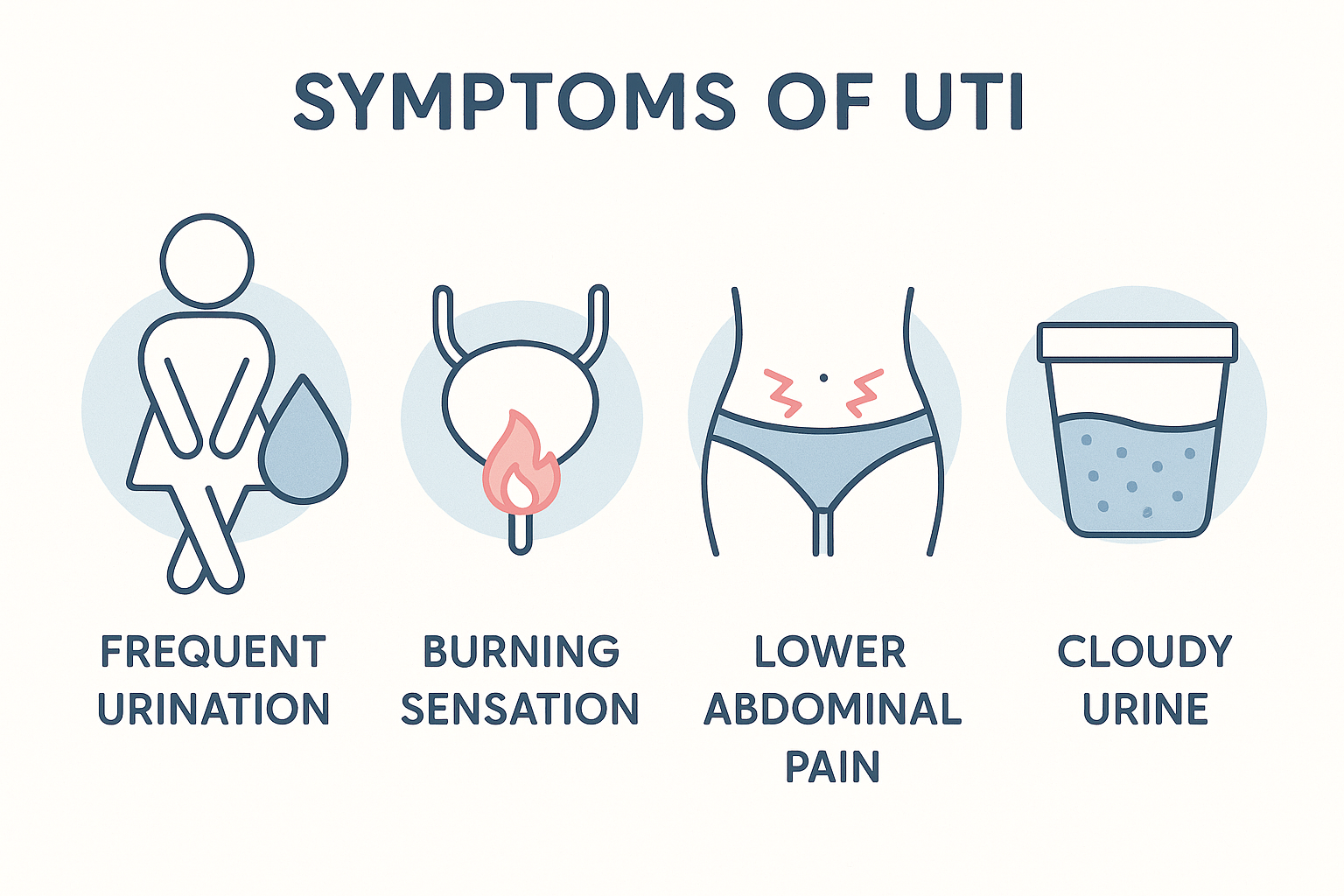
Common UTI Symptoms
Recognizing UTI symptoms early can help you seek timely treatment. Here are the most common signs:
- A persistent urge to urinate, even if little comes out
- Burning sensation or pain while urinating
- Cloudy, dark, or strong-smelling urine
- Frequent urination in small amounts
- Blood in urine (hematuria)
- Pelvic pain or discomfort in women
- In severe cases: fever, chills, nausea, or back pain (indicating a kidney infection)
If you notice any of these UTI symptoms, it’s important not to ignore them. Early detection ensures faster recovery.
UTI Causes
A UTI occurs when bacteria, usually E. coli, enter the urinary tract. Several factors increase the risk of UTI infection:
- Poor personal hygiene
- Sexual activity (especially with new partners)
- Use of certain contraceptives like spermicides or diaphragms
- Hormonal changes during pregnancy or menopause
- Holding urine for long periods
- Dehydration (not drinking enough water)
- Medical conditions such as diabetes or kidney stones
- Weakened immune system
Understanding these UTI causes can help in reducing your chances of infection.
UTI Treatment Options
If you suspect a UTI infection, visiting a doctor is essential. A healthcare professional will recommend UTI treatment based on the severity of your condition:
1. Antibiotics
The most common UTI treatment, prescribed for bacterial infections. It’s important to complete the full course even if symptoms improve.
2. Increased Fluid Intake
Drinking plenty of water helps flush bacteria from the urinary tract.
3. Pain Relief
Over-the-counter medications may be prescribed to ease discomfort and burning sensation.
If untreated, UTIs can spread to the kidneys and become serious, making early UTI treatment crucial.
When to See a Doctor
Seek medical attention if:
- Symptoms persist for more than 2 days
- You notice blood in your urine
- You experience fever, chills, or severe back pain
- You have recurring UTIs (multiple infections within a year)
A doctor can provide personalized UTI treatment to prevent further complications.
How to Prevent UTI Infection
Prevention is always better than cure. Here are some effective ways to lower your risk:
- Stay hydrated drink 8–10 glasses of water daily
- Don’t hold urine for long periods
- Wipe front to back after using the toilet
- Urinate after sexual intercourse
- Wear breathable cotton underwear
- Avoid harsh feminine hygiene products that disrupt natural balance
These simple steps can help reduce the likelihood of UTI infection and improve overall urinary health.
FAQs on UTIs
1. What is the fastest way to cure a UTI?
The fastest way is through prescribed antibiotics. Drinking water and resting help speed up recovery.
2. Can a UTI go away on its own?
Mild cases might resolve, but most UTIs require treatment. Ignoring symptoms can lead to complications.
3. What foods should I avoid with a UTI?
Avoid caffeine, alcohol, artificial sweeteners, and spicy foods as they may irritate the bladder.
4. How do I know if my UTI is serious?
If you experience fever, back pain, nausea, or blood in your urine, seek immediate medical help it may have spread to the kidneys.
5. Are UTIs contagious?
No, UTIs are not contagious. However, sexual activity can increase the risk of infection.
Conclusion: Why Choose Us?
Choose Care For Her as your trusted partner in women’s health. Led by Dr. Anuja Ojha, a dedicated and compassionate obstetrician and gynecologist, we offer personalized care through every stage of womanhood from adolescence to pregnancy, and beyond.
Our patient-first approach ensures you receive empathetic guidance, advanced medical expertise, and holistic care in a comfortable environment. Whether it’s routine check-ups, fertility consultations, or pregnancy care, we’re here to support your journey with trust and transparency.
To learn more, contact us at 7400424637 or visit www.careforher.in