Understanding the Importance of a Pelvic Exam
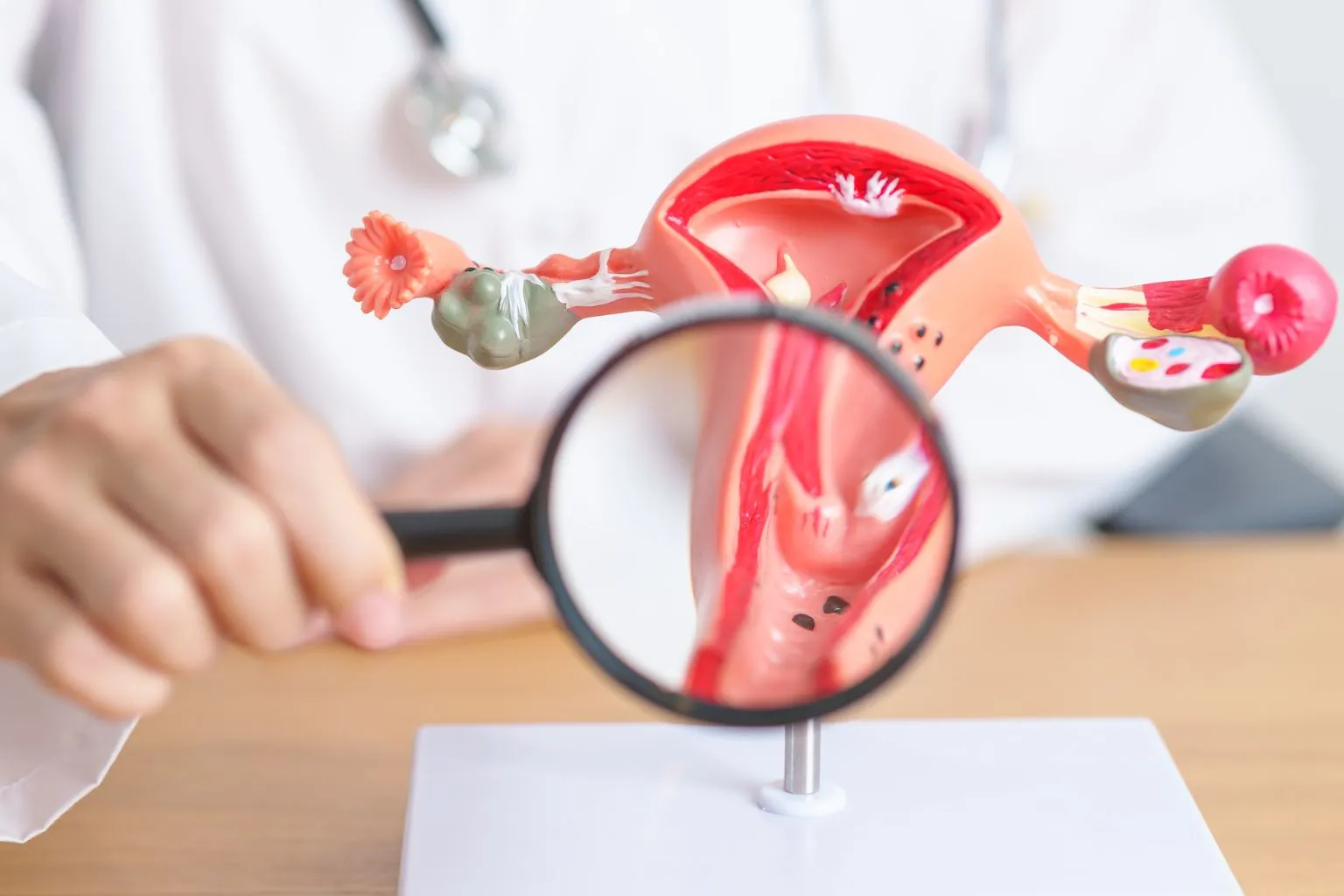
Many women feel nervous when they hear the term “pelvic exam,” but it’s one of the most important ways to maintain reproductive and overall health. A pelvic exam helps your gynecologist check the health of your uterus, ovaries, cervix, and vagina. It’s a routine part of women’s health care and can help detect early signs of infections, cysts, fibroids, or even cancers.
If you’ve ever wondered what is a pelvic exam or when you should get one, this guide will explain everything you need to know in simple and reassuring language. Dr. Anuja Ojha and the team at Care For Her believe that understanding your body is the first step toward taking control of your health.
What is a Pelvic Exam?
A common question many women have is: what is a pelvic exam? A pelvic exam is a medical check-up where your gynecologist examines your reproductive organs to make sure everything is healthy. The exam helps identify any abnormalities, infections, or issues that may need attention.
During a pelvic exam, your doctor will visually and physically check the vagina, cervix, uterus, fallopian tubes, ovaries, and sometimes the bladder and rectum. It usually takes only a few minutes and is a vital part of preventive women’s health care.
To put it simply, if you are wondering what is a pelvic exam it’s a quick, safe, and important procedure to help detect health problems early, even before symptoms appear.
Why is a Pelvic Exam Important?
A pelvic exam is more than just a routine test it’s a powerful tool for maintaining women’s health. Regular pelvic exams help your gynecologist:
- Detect infections like yeast or bacterial vaginosis
- Screen for sexually transmitted infections (STIs)
- Identify abnormal growths such as fibroids or cysts
- Check for early signs of cervical or ovarian cancer
- Evaluate symptoms such as pelvic pain, unusual discharge, or irregular bleeding
Even if you’re not experiencing any symptoms, a yearly pelvic exam ensures that your reproductive organs remain healthy. Early detection through a pelvic exam can lead to timely treatment and better outcomes.
When Should You Get a Pelvic Exam?
The right time to begin pelvic exams can vary depending on your age, health history, and symptoms. In general:
- Most women should start pelvic exams around the age of 21 or when they become sexually active.
- Women over 30 should continue getting regular exams as part of their preventive health check-ups.
- You should schedule an exam immediately if you experience symptoms such as pelvic pain, irregular periods, unusual discharge, or bleeding after intercourse.
For pregnant women, a pelvic exam may also be recommended at different stages to monitor cervical changes and ensure a healthy pregnancy.
What Happens During a Pelvic Exam?
Understanding the process can make your experience more comfortable. Here’s what typically happens during a pelvic exam:
- Preparation: You’ll be asked to lie down on an examination table with your feet placed in stirrups. Your doctor will ensure you feel relaxed and explain each step before proceeding.
- External Examination: The gynecologist first examines the external genital area to check for swelling, sores, or irritation.
- Speculum Examination: A sterile medical instrument called a speculum is gently inserted into the vagina. This allows the doctor to see the vaginal walls and cervix clearly.
- Pap Smear (if required): During this stage, a small sample of cervical cells may be collected to test for infections or early signs of cervical cancer.
- Internal (Bimanual) Examination: The doctor will insert two gloved fingers into the vagina while pressing on your lower abdomen with the other hand. This helps check the size, shape, and position of the uterus and ovaries.
The entire pelvic exam usually lasts just a few minutes. You might feel slight pressure or discomfort, but it should not be painful. If you ever feel pain, you should inform your doctor right away.
How to Prepare for a Pelvic Exam
You don’t need any special preparation for a pelvic exam, but a few simple steps can make the experience smoother:
- Schedule your exam when you are not on your period, unless it’s urgent.
- Avoid sexual intercourse, vaginal creams, or douching for 24 hours before the exam.
- Empty your bladder before the appointment to feel more comfortable.
- Relax and communicate with your doctor if you feel nervous your comfort and safety are the top priority.
Being well-informed about what is a pelvic exam can help you feel confident and in control during the process.
Common Concerns and Myths About Pelvic Exams
Many women delay or avoid pelvic exams due to anxiety or misconceptions. Let’s clear up some common myths:
- Myth 1: Pelvic exams are painful.
In reality, most pelvic exams are not painful, though mild discomfort is normal. Skilled gynecologists like Dr. Anuja Ojha use gentle techniques to ensure the process is as comfortable as possible. - Myth 2: You only need a pelvic exam if you have problems.
This is not true. Regular pelvic exams are preventive, helping detect issues before they cause noticeable symptoms. - Myth 3: You can skip a pelvic exam after menopause.
Even after menopause, it’s important to continue pelvic exams to monitor vaginal health, hormone changes, and screen for cancers or infections.
Clearing these misconceptions helps more women understand the importance of regular check-ups and feel at ease during their appointments.
What Do the Results Mean?
After the pelvic exam, your doctor will explain the findings. In most cases, results are normal, meaning your reproductive organs are healthy. If there are any concerns such as infections, cysts, or abnormal Pap smear results, your doctor may recommend additional tests or treatment.
Regular pelvic exams ensure that any potential issues are caught early and managed effectively. It’s always better to address minor problems before they develop into more serious conditions.
When to See Your Gynecologist
Even if your previous pelvic exam was normal, you should book an appointment with your gynecologist if you experience:
- Persistent pelvic or lower abdominal pain
- Unusual vaginal discharge or odor
- Irregular menstrual cycles
- Pain during intercourse
- Bleeding after sex or between periods
These symptoms can indicate infections, hormonal imbalances, or other underlying conditions that require medical attention.
Summary / Takeaway
A pelvic exam is an essential part of women’s healthcare, helping to maintain reproductive health, detect infections early, and monitor changes in the uterus, cervix, and ovaries. If you’ve ever wondered what is a pelvic exam, it’s simply a routine, safe, and vital procedure designed to keep you healthy.
Regular pelvic exams are not just for when something feels wrong they are a preventive measure that ensures peace of mind and early detection of potential health concerns.
If you’re due for your next pelvic exam or have questions about your reproductive health, Dr. Anuja Ojha at Care For Her offers gentle, expert care in a supportive environment.
Why Choose Us
Choose Care For Her as your trusted partner in women’s health. Led by Dr. Anuja Ojha, a dedicated and compassionate obstetrician and gynecologist, we provide personalized care through every stage of womanhood from adolescence to pregnancy, and beyond. Our patient-first approach ensures you receive empathetic guidance, advanced medical expertise, and holistic care in a comfortable setting. Whether it’s preventive check-ups, fertility consultations, or pregnancy care, we’re here to support your journey with trust and transparency.
To learn more, contact us at 7400424637 or visit www.careforher.in