Sexual health is an essential part of overall well-being, yet it is often overlooked due to stigma or lack of awareness. Understanding STI and how it affects women is crucial for early diagnosis, treatment, and prevention. In this blog, we will break down what is sexually transmitted infections, their symptoms, testing options, and sexually transmitted infection treatment in a simple, clear manner.
What Is STI (Sexually Transmitted Infection)?
STI refers to infections that are primarily spread through sexual contact, including vaginal, oral, or anal sex. These infections are caused by bacteria, viruses, or parasites and can affect anyone who is sexually active.
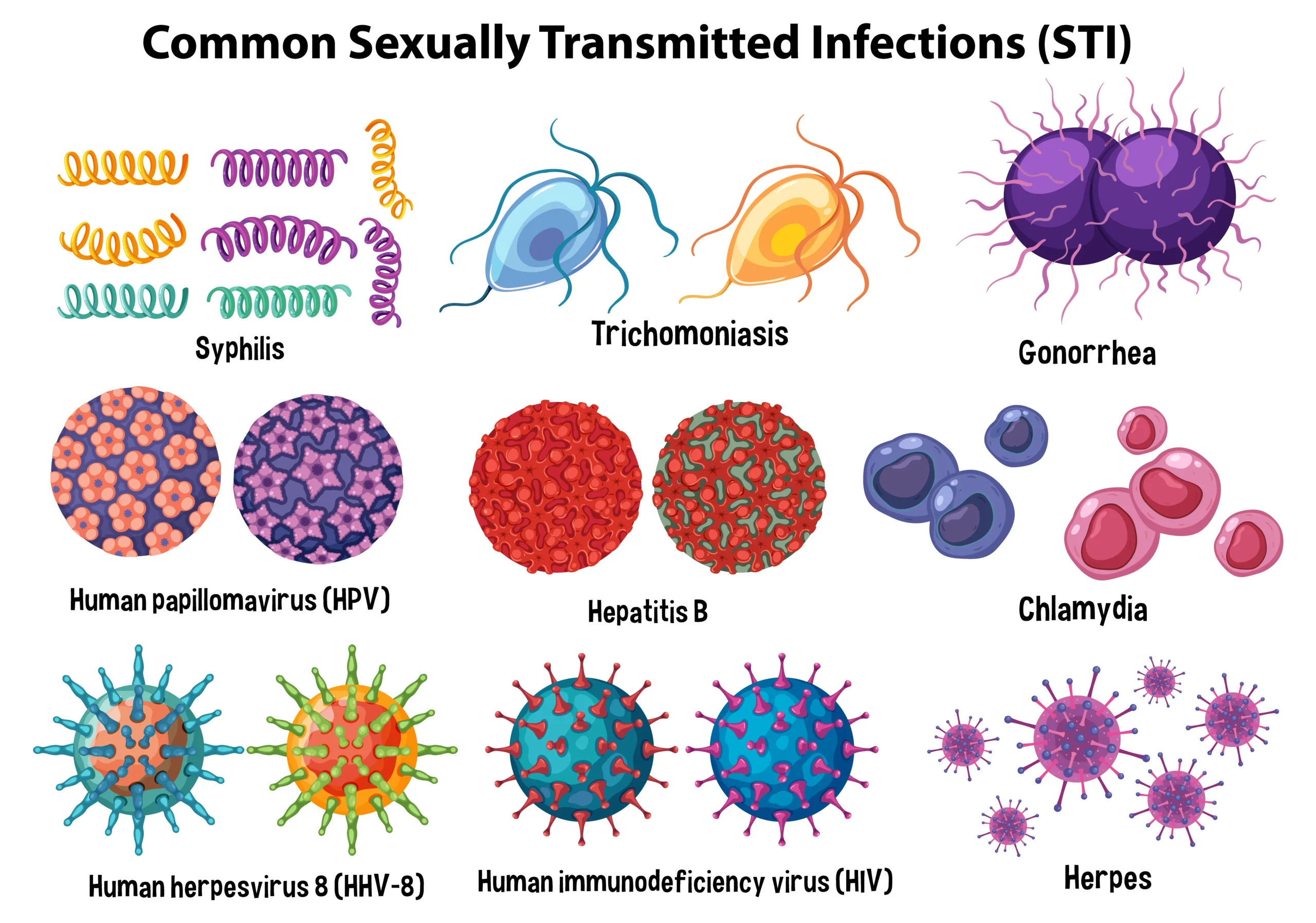
When we talk about what is sexually transmitted infections, we are referring to a wide range of conditions such as chlamydia, gonorrhea, human papillomavirus (HPV), herpes, and HIV. Many sexually transmitted infections may not show symptoms initially, making regular screening extremely important.
Understanding what is sexually transmitted infections helps women take proactive steps toward maintaining reproductive and overall health.
Common Sexually Transmitted Infections in Women
Sexually transmitted infections in women can sometimes present differently than in men. In many cases, women may experience subtle or no symptoms, which increases the risk of complications if left untreated.
Some common sexually transmitted infections in women include:
- Chlamydia
- Gonorrhea
- HPV (Human Papillomavirus)
- Herpes Simplex Virus
- HIV/AIDS
- Trichomoniasis
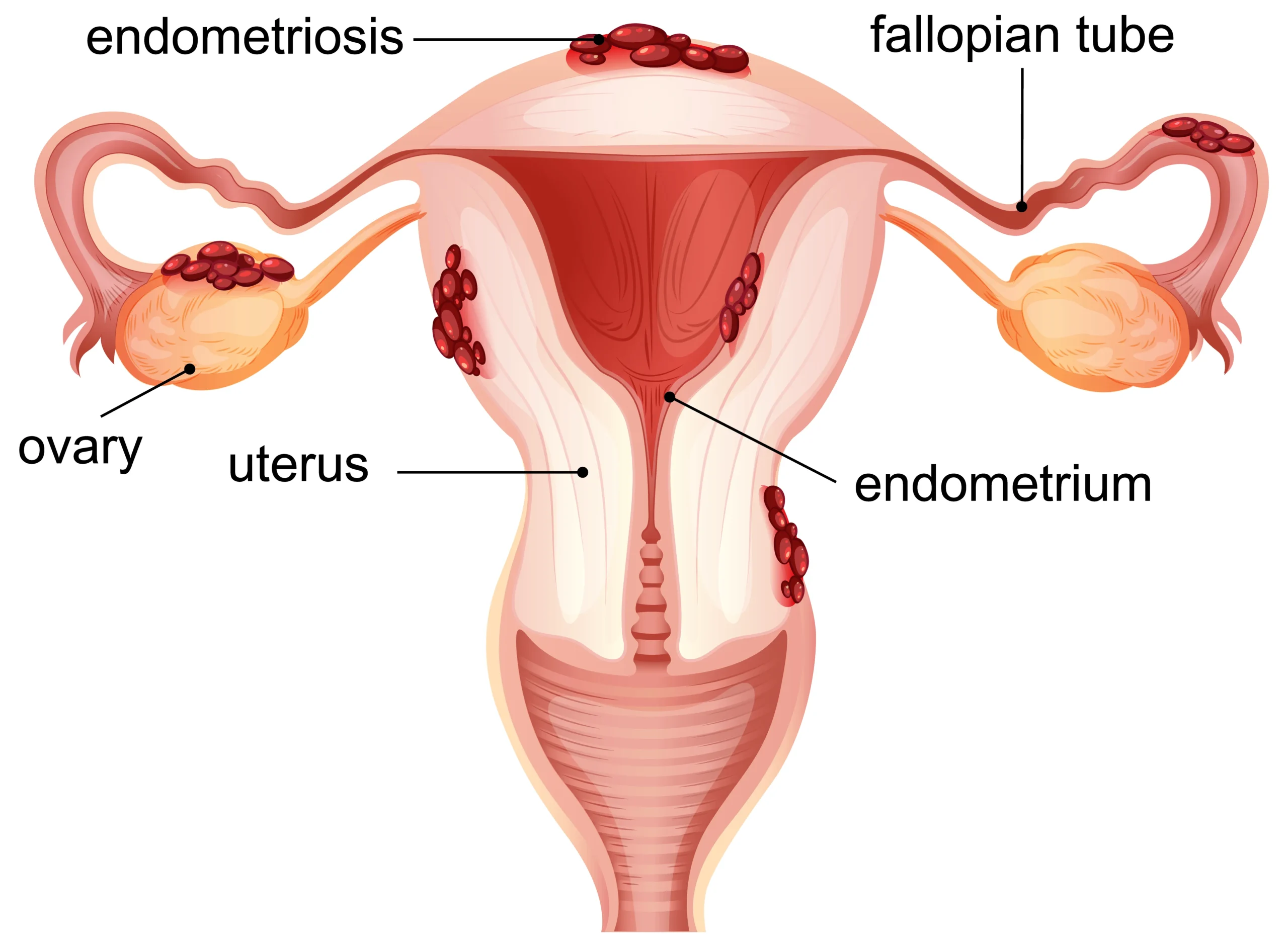
Sexually transmitted infections in women can affect the reproductive system and may lead to conditions like pelvic inflammatory disease (PID), infertility, or complications during pregnancy if not treated on time.
Signs of Sexually Transmitted Infections
Recognizing the signs of sexually transmitted infections is key to early diagnosis and treatment. However, it is important to note that many STI cases may be asymptomatic.
Common signs of sexually transmitted infections include:
- Unusual vaginal discharge
- Burning sensation during urination
- Pain during intercourse
- Lower abdominal pain
- Sores, bumps, or rashes in the genital area
- Irregular bleeding between periods
Since these signs of sexually transmitted infections can overlap with other conditions, it is essential to consult a gynecologist for proper diagnosis.
How Are Sexually Transmitted Infections Diagnosed?
Early detection plays a major role in managing sexually transmitted infections. Testing is simple, confidential, and widely available.
Diagnosis methods include:
- Blood tests (for HIV, syphilis)
- Urine tests (for chlamydia and gonorrhea)
- Swab tests from the cervix or vagina
- Pap smear (for detecting HPV-related changes)
Women who are sexually active, have multiple partners, or are planning pregnancy should consider regular STI screening. Timely diagnosis of sexually transmitted infections in women helps prevent long-term complications.
Sexually Transmitted Infection Treatment Options
Sexually transmitted infection treatment depends on the type of infection.
- Bacterial infections (like chlamydia and gonorrhea) are treated with antibiotics
- Viral infections (like herpes and HIV) are managed with antiviral medications
- Parasitic infections (like trichomoniasis) are treated with specific medications
Sexually transmitted infection treatment is most effective when started early. It is also important that both partners get treated to avoid reinfection.
Completing the full course of prescribed medication is crucial for successful sexually transmitted infection treatment.
Can STI Be Prevented?
Yes, STI prevention is possible with the right precautions:
- Use protection such as condoms during sexual activity
- Maintain a mutually monogamous relationship
- Get vaccinated (HPV vaccine)
- Undergo regular screenings
- Avoid sharing personal hygiene items
Being informed about sexually transmitted infections and taking preventive steps can significantly reduce the risk.
When Should You See a Doctor?
You should consult a gynecologist if you:
- Notice any unusual symptoms
- Have had unprotected sex
- Have multiple sexual partners
- Are planning a pregnancy
- Have a partner diagnosed with STI
Even if you feel completely fine, routine screening for sexually transmitted infections is recommended for sexually active women.
FAQs
-
What is STI and how does it spread?
STI refers to infections transmitted through sexual contact. They spread via vaginal, oral, or anal sex with an infected partner.
-
Are sexually transmitted infections always symptomatic?
No, many sexually transmitted infections may not show symptoms, especially in women, which is why regular testing is important.
-
How often should women get tested for STI?
Sexually active women should get tested at least once a year, or more frequently if they have multiple partners.
-
Can sexually transmitted infections in women affect fertility?
Yes, untreated sexually transmitted infections in women can lead to pelvic inflammatory disease and infertility.
-
Is sexually transmitted infection treatment effective?
Yes, most sexually transmitted infection treatment options are highly effective, especially when diagnosed early.
-
Can STI be cured completely?
Some STI, like bacterial infections, can be cured. Viral infections can be managed but may not be completely eliminated.
-
Is it safe to get pregnant if I have an STI?
It depends on the type of infection. Proper sexually transmitted infection treatment and medical guidance are necessary before planning pregnancy.
Why Choose Us?
Choose Care For Her as your trusted partner in women’s health. Led by Dr. Anuja Ojha, a dedicated and compassionate obstetrician and gynecologist, we offer personalized care through every stage of womanhood from adolescence to pregnancy, and beyond. Our patient-first approach ensures you receive empathetic guidance, advanced medical expertise, and holistic care in a comfortable environment. Whether it’s routine check-ups, fertility consultations, or pregnancy care, we’re here to support your journey with trust and transparency. To learn more, contact us at 7400424637 or visit www.careforher.in